Men's Health & Wellness Biomarkers Explained
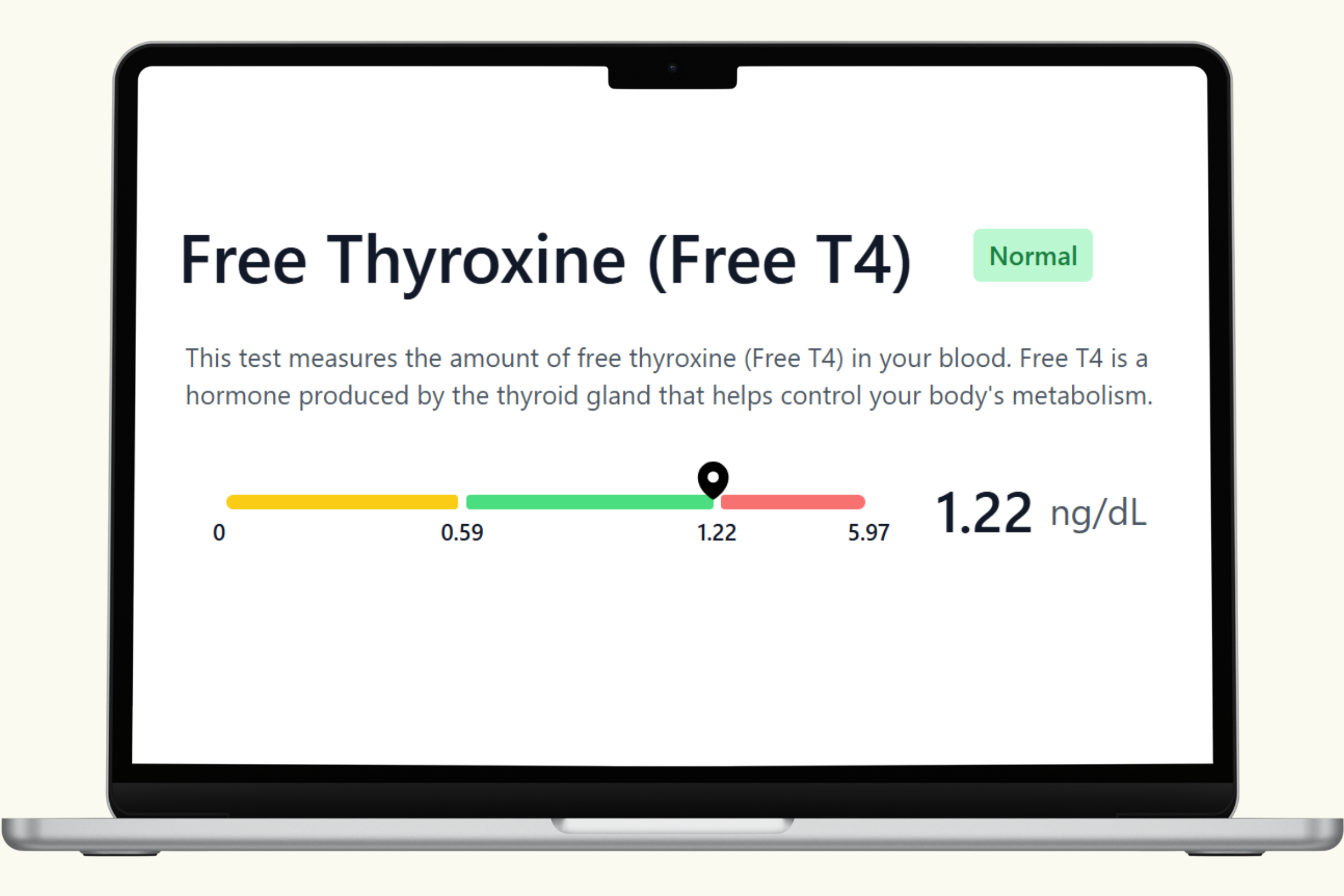
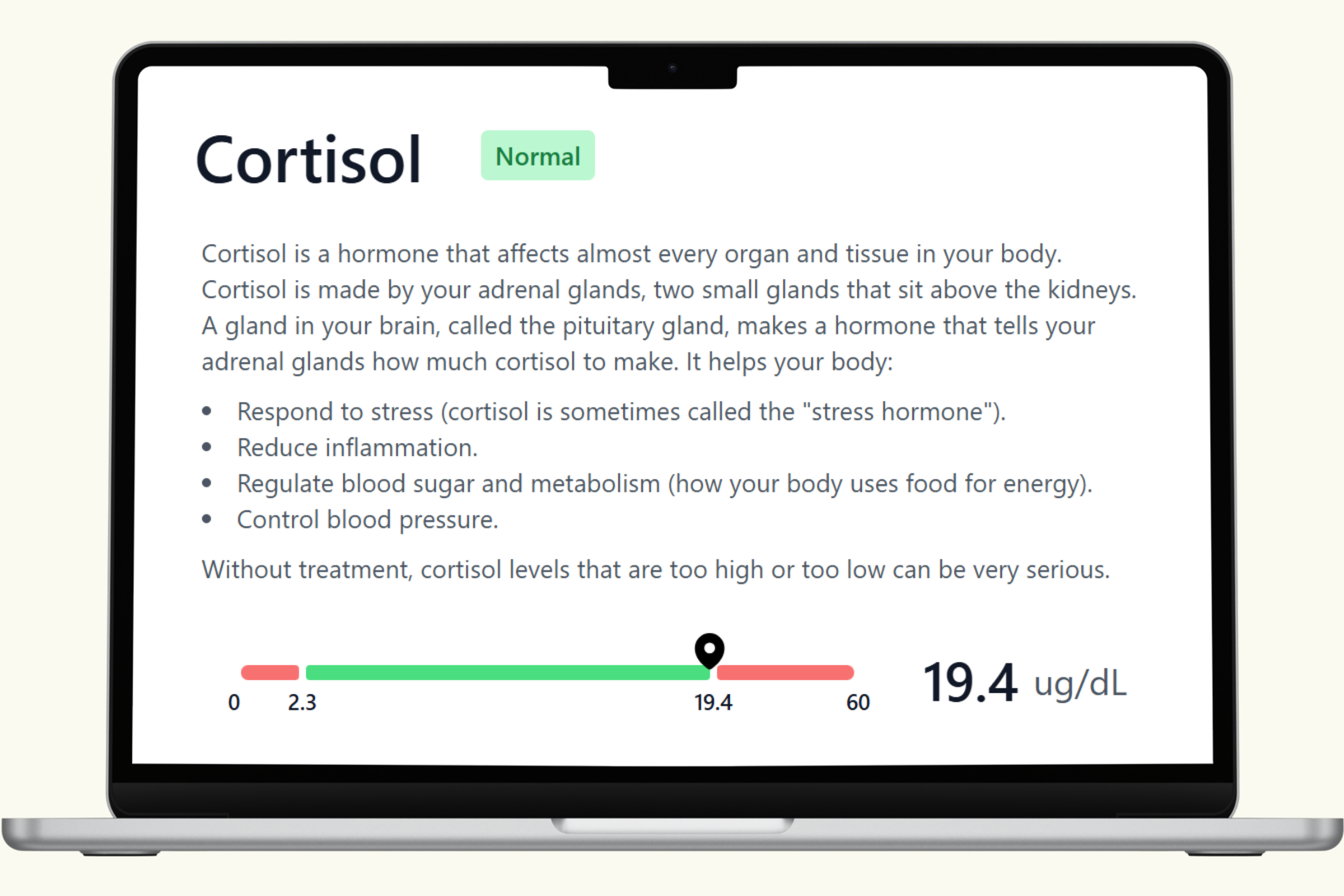
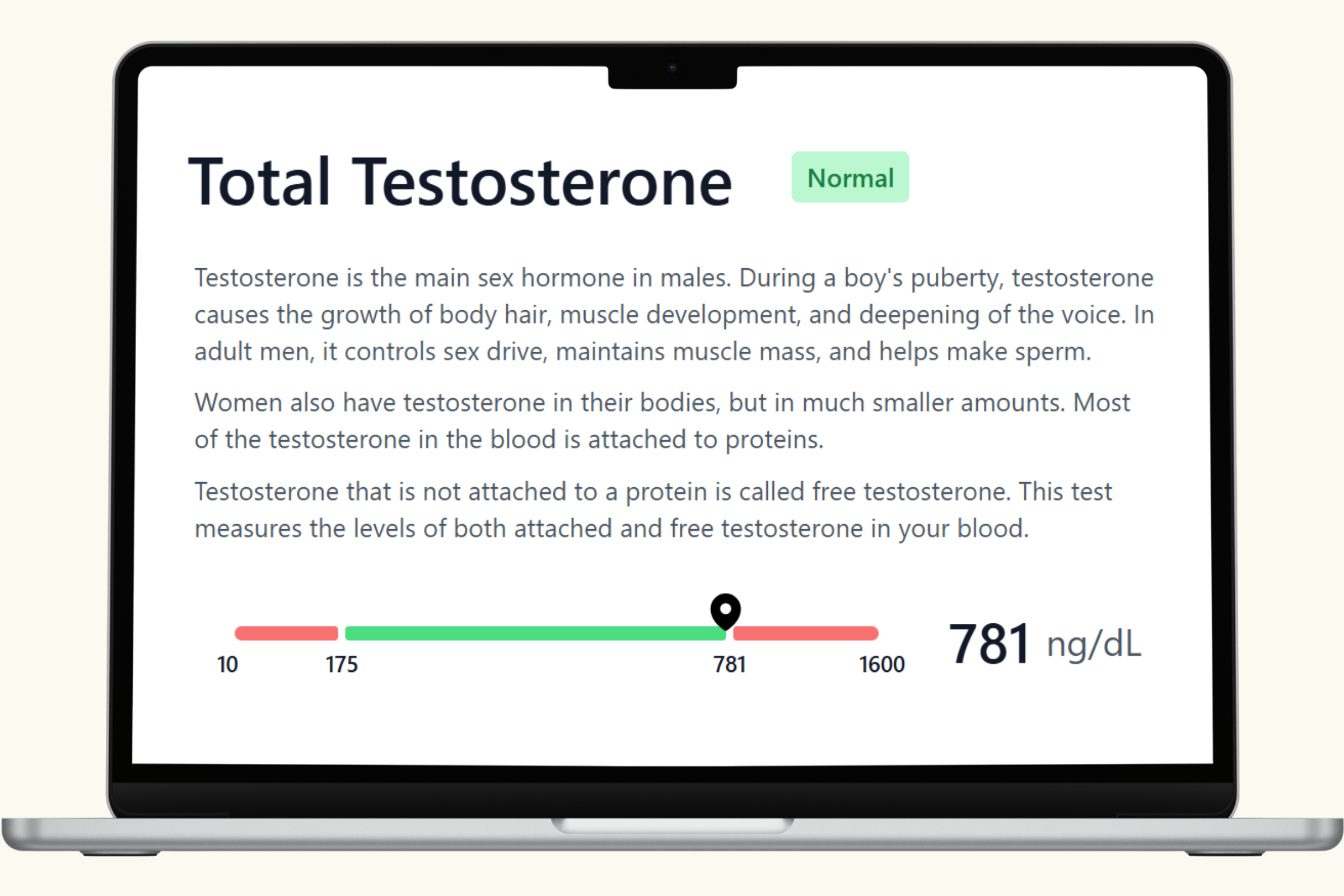
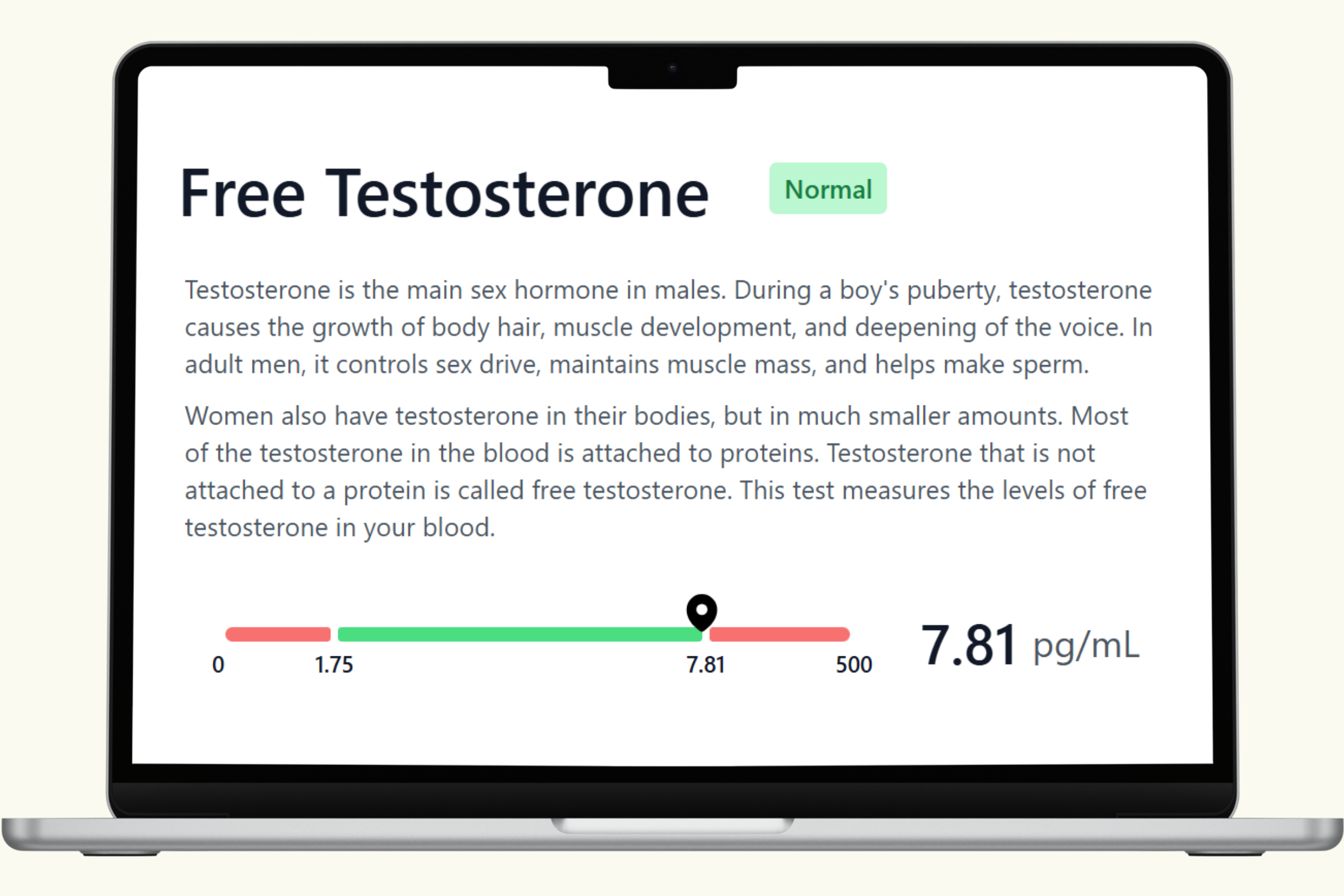
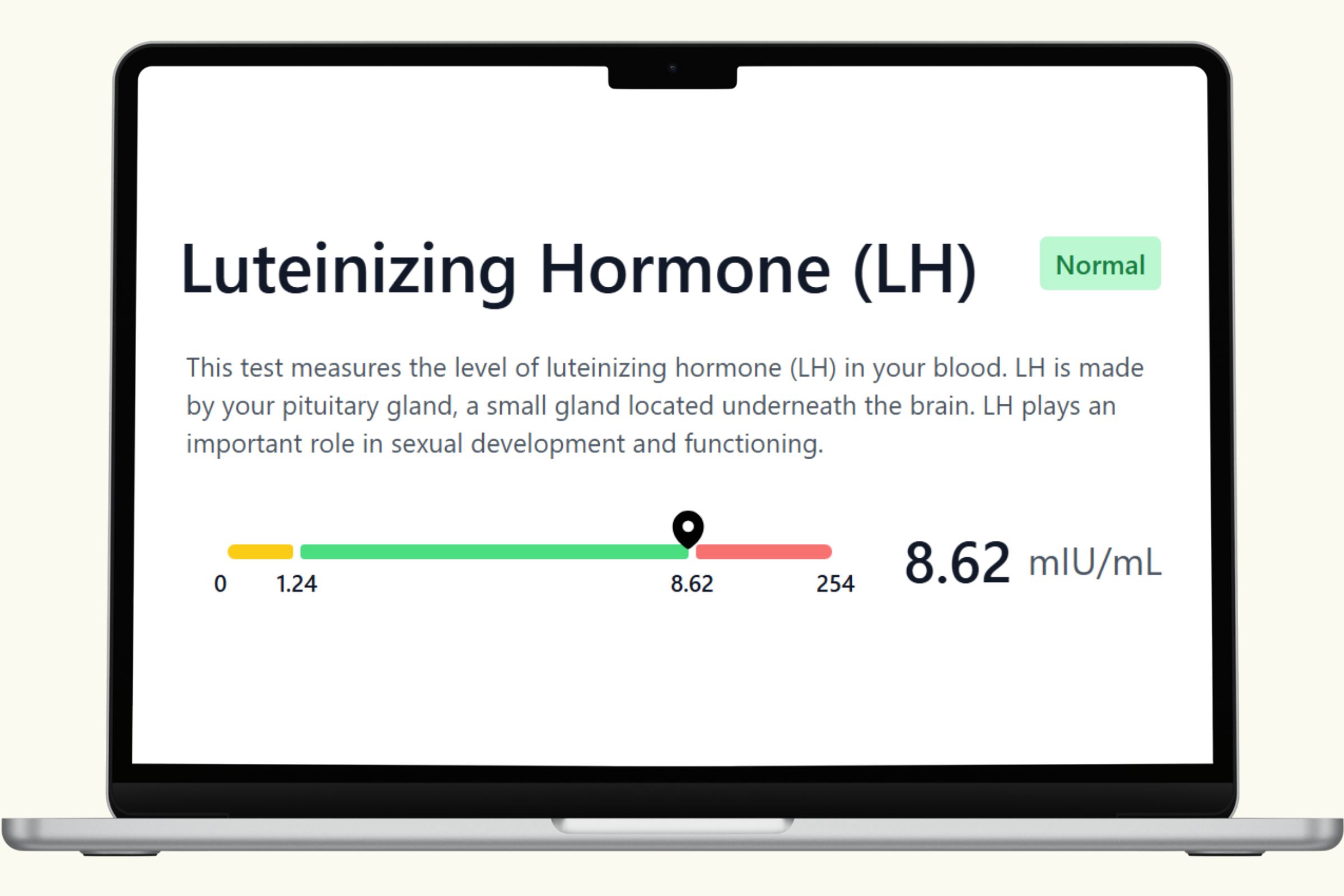
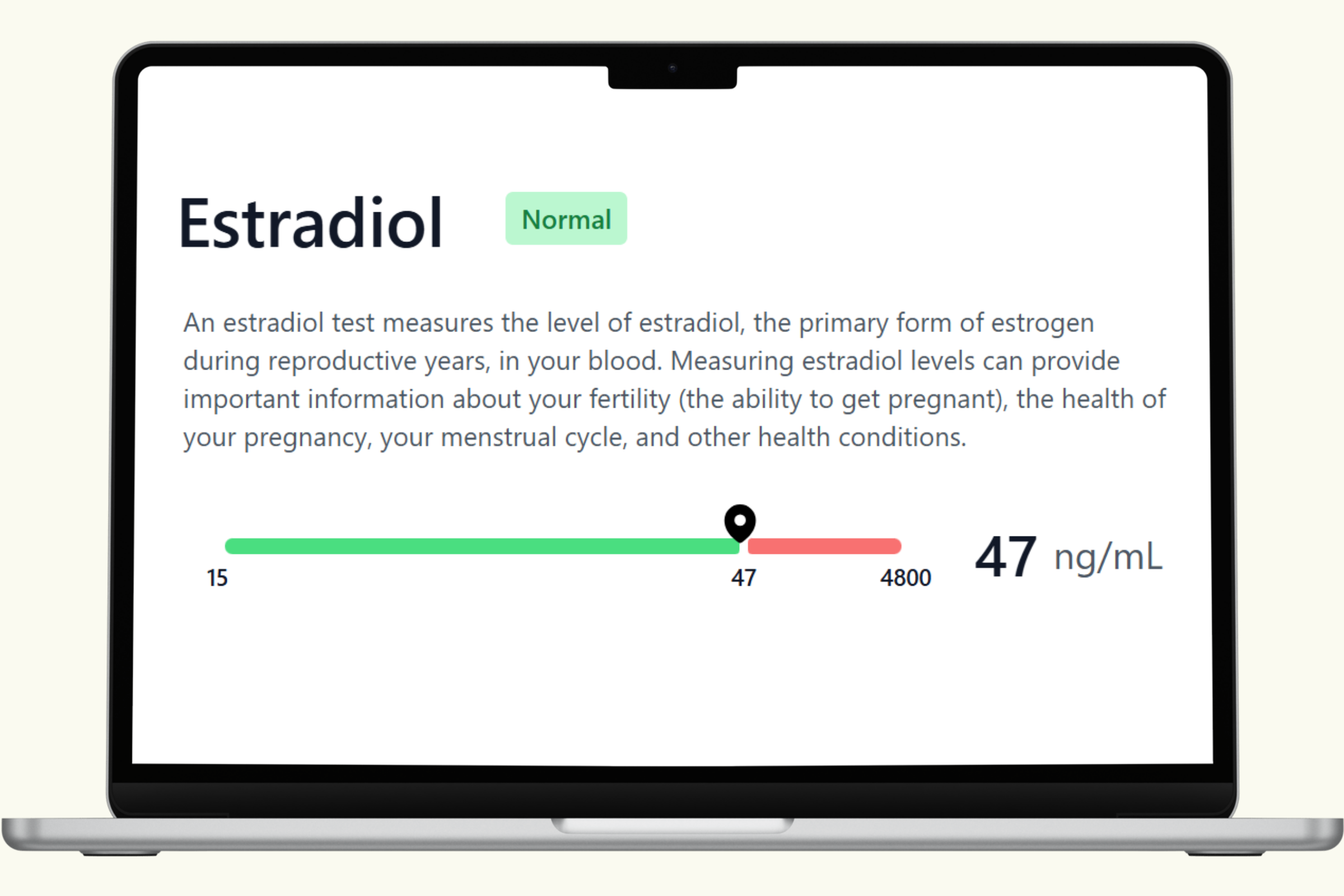
A comprehensive men's health blood panel gives you a current snapshot of the systems that matter most: testosterone and hormonal balance, cardiovascular function, metabolic health, thyroid status, and key nutrient levels. These biomarkers don't just report numbers — they reveal how your body is functioning right now across multiple interconnected systems.
This hub covers each biomarker in the PlexusDx Men's Health & Wellness Blood Test in detail — what it measures, what influences it, and how it connects to overall wellness. Results are delivered through your PlexusDx Results Portal within 1–2 business days, with personalized guidance based on your individual levels.
For deeper insight, many customers pair blood results with the Precision Functional Health Genetic Test to see both current biomarker status and long-term genetic tendencies in the same Results Portal.
No doctor's order required. HSA/FSA eligible.