Nutrition Deficiency Biomarkers Explained
Nutritional deficiencies are far more common than most people realize — and they're often silent. Suboptimal levels of key vitamins and minerals can affect energy, immune function, bone health, mood, and metabolic performance long before obvious symptoms appear. The only way to know your current status is to measure it.
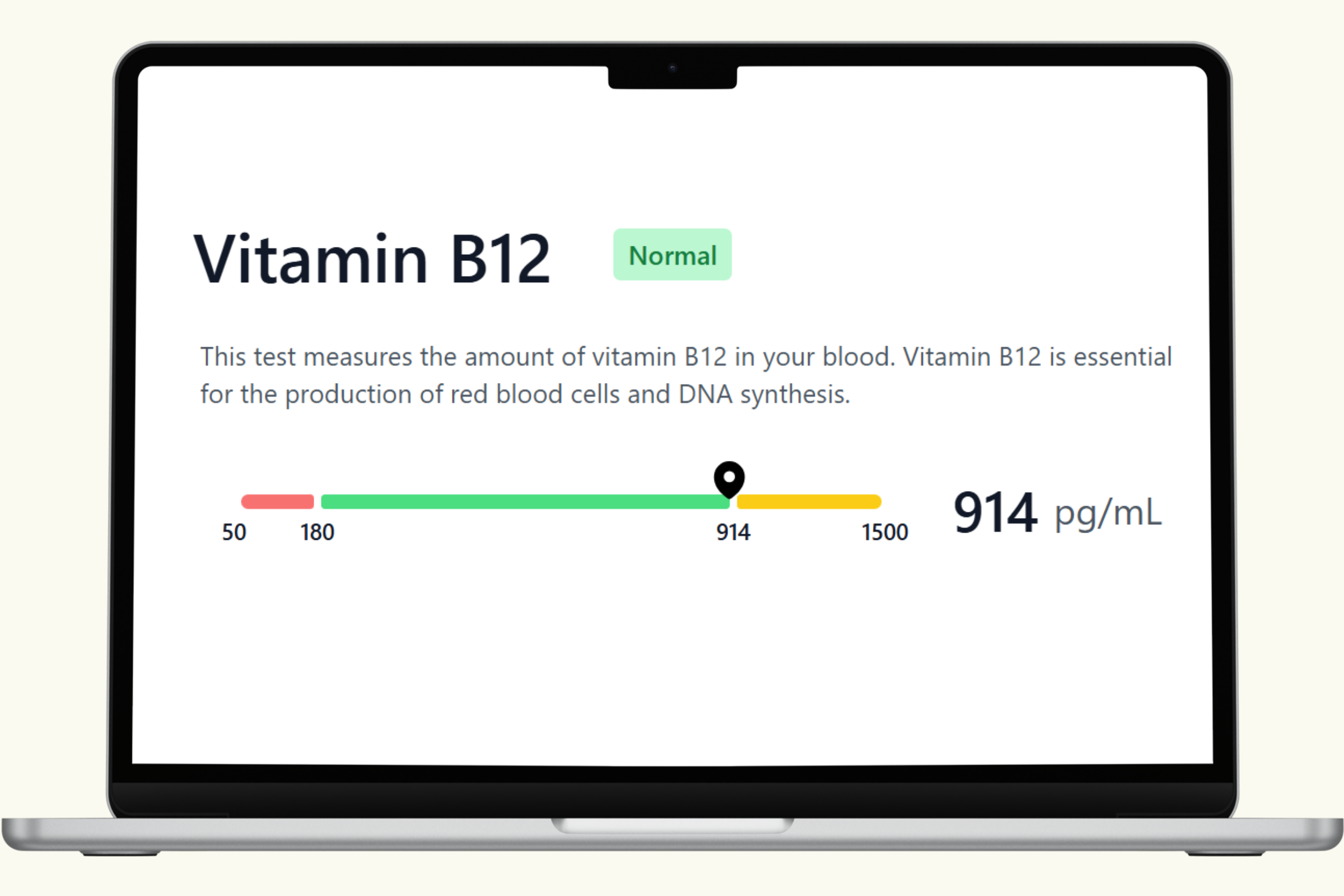
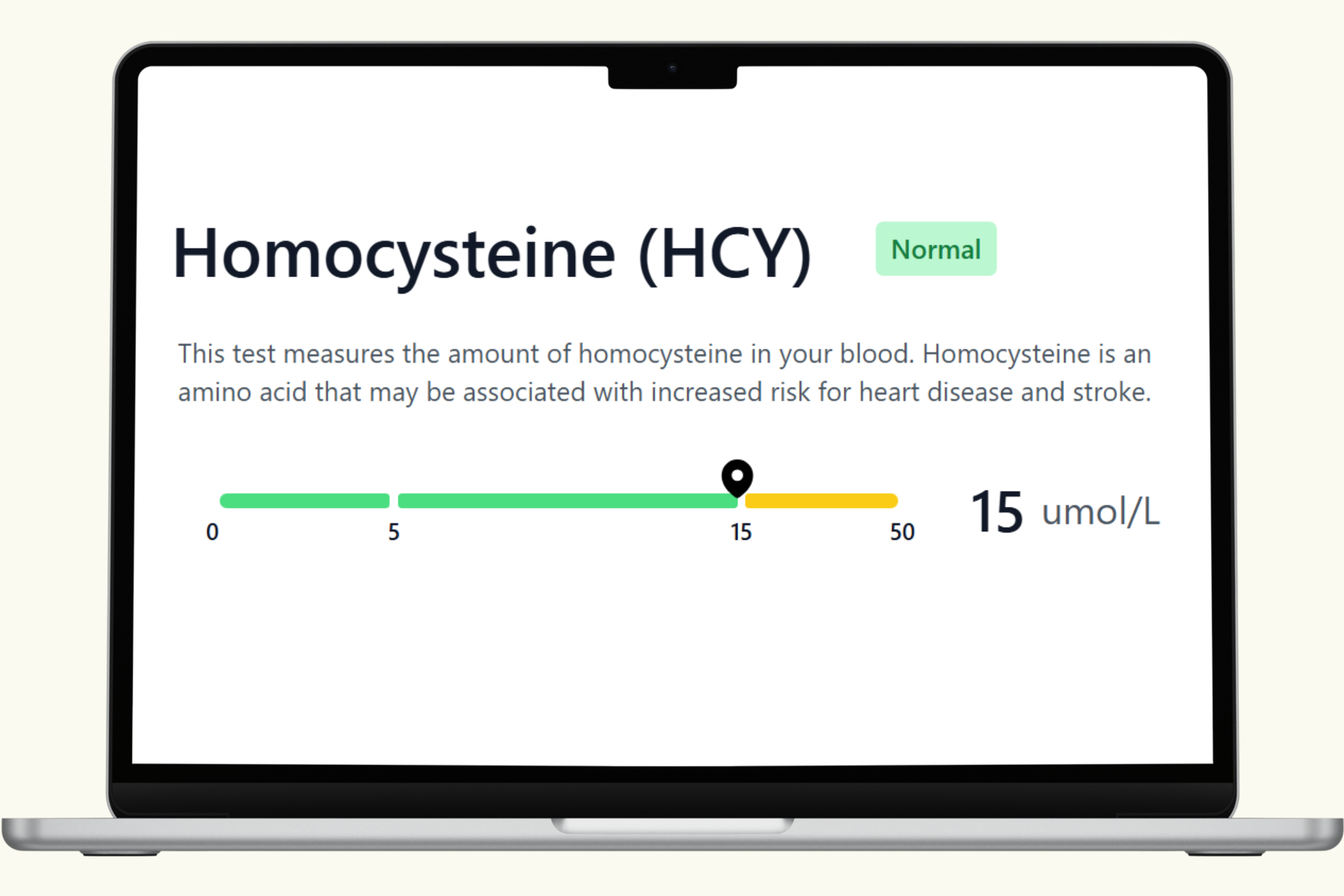
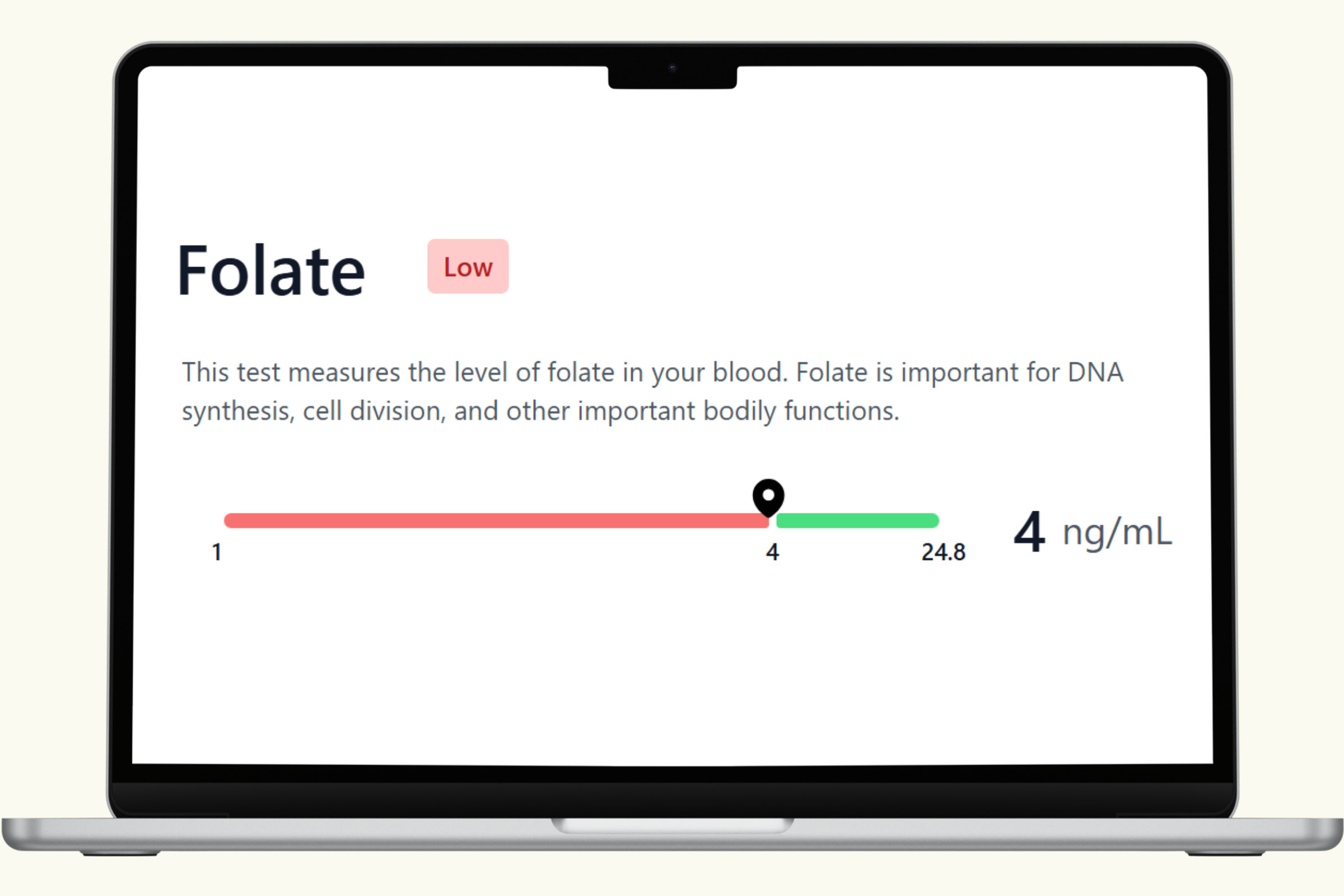
This hub covers each biomarker in the PlexusDx Nutrition Deficiency Blood Test — explaining what each nutrient does, what low or suboptimal levels look like in practice, and what dietary and supplement strategies support optimal levels. Results are delivered through your Results Portal within 1–2 business days with personalized guidance.
For a complete nutritional picture, many customers pair blood results with the Precision Diet & Weight Loss Genetic Test to understand both current nutrient status and long-term genetic influences on nutrient absorption.
No doctor's order required. HSA/FSA eligible.